'A life sentence': The frightening trend emerging in young coronavirus patients
Roughly six months into the global coronavirus pandemic a disturbing picture is beginning to emerge of the long-term impact the virus can have on young and once healthy people.
Doctors and researchers in the US – where the virus continues to spread in much of the country – are sounding the alarm about a growing group of people who are presenting with debilitating symptoms of Myalgic Encephalomyelitis (ME), better known as Chronic Fatigue Syndrome.
The disease, which includes a hugely diverse range of symptoms, is notoriously difficult to assess and diagnose making it difficult for patients to get recognition, let alone effective treatment.
As a result, the flood of coronavirus patients still experiencing devastating health effects months on have gathered in groups online where they share experiences, compare notes and vent their frustrations.
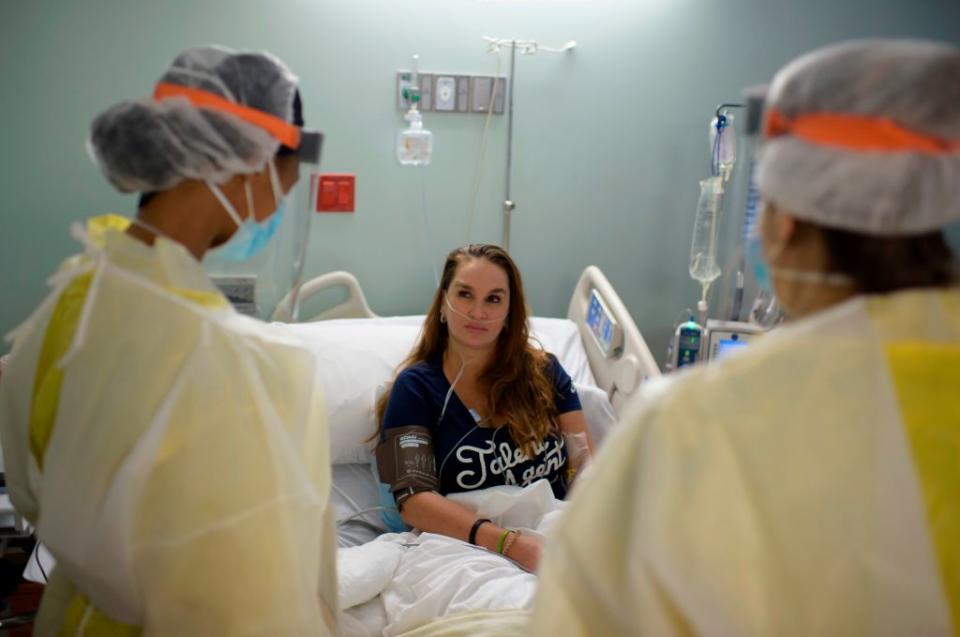
In contrast to the common perception of COVID-19 affecting older people more adversely, those who appear to be developing ME-like symptoms are often young.
The disease is typically brought on by some sort of viral infection due to a response known as a cytokine storm, where the body starts to attack its own cells and tissues rather than just fighting off the virus.
“For whatever reason in some patients this response just seems to get out of control,” says Oved Amitay, Chief Executive Officer at the Solve ME/CFS Initiative in the US.
“It actually tends to be the younger population who are affected by this,” he told Yahoo News Australia.
“These are not necessarily patients who are hospitalised [but] they are the group that seems to be most affected.”

In lieu of a vaccine, we’re still in the early stages of the SARS-CoV-2 pandemic. And while it takes more than six months of symptoms before a patient will likely receive a diagnosis of ME, the longer-term consequences of COVID-19 are starting to become better understood.
A recent study of coronavirus patients carried out by the US Centers for Disease Control (CDC), found that 35 per cent of patients were still experiencing symptoms up to three weeks after testing positive. While a small study published in the medical journal Lancet last week found 55 per cent of patients surveyed were still displaying neurological symptoms during follow-up visits three months after being diagnosed.
“Every day that goes by, we learn more of those stories,” Mr Amitay said.
Patient ‘scared my body is shutting down’
Support groups have cropped up on social media filled with desperate posts of people trying to understand how long they can expect to suffer ongoing symptoms as they swap stories of “Long Covid”.
One private Facebook group, named the Long Covid Support Group, has 17,000 members and counting and is filled with people who have come to identify as coronavirus long-haulers. Some have ongoing symptoms more than four months after contracting the virus.
They report dealing with immense fatigue, trouble sleeping, muscle aches, fever, loss of cognitive function, gastrointestinal issues, severe headaches, brain fog, skin rashes, a sensitivity to noise and light and a myriad of other symptoms.
'Dying not only worry': Coronavirus 'long-hauler' details horrific symptoms
Melbourne's 'magic number': When is it safe for the city to leave lockdown?
Coronavirus: Aussies told to 'cancel their holiday Christmas plans'
Many report feeling better, only for symptoms to return suddenly weeks later – something that is a hallmark of ME, says Emily Taylor, the Director of Advocacy at the Solve ME/CFS Initiative.
She has experienced the disease first hand after spending years looking after her mother who is afflicted by it.
“Symptoms can come and go without warning,” she told Yahoo News Australia. “She can wake up one morning and be suddenly unable to use her legs.
“For some patients this is a life sentence, this is their new normal.”
When it comes to ME/CFS, it affects women far more than men – at a rate of about four to one. While it’s too early to tell if the symptoms triggered by COVID-19 will follow a similar trend, it appears somewhat likely, Ms Taylor said.
Coronavirus long-haulers create ‘scientific opportunity’
For researchers and medical professionals who work in the chronic disease field, the fact that the novel coronavirus has sparked these long-term symptoms did not come as a surprise.
“It is not scientifically surprising,” Ms Taylor said. “We were kind of on guard.”
Because Chronic Fatigue Syndrome still lacks a specific disease criteria and is difficult to diagnose (and has no proven cure), it’s hoped the wave of coronavirus long-haulers could help the medical field better understand the disease and its onset.
“It’s probably the best scientific opportunity to study this,” Mr Amitay said.
He has dedicated most of his professional career to the development of life-changing therapeutic options for people affected by rare genetic diseases.
“With the coronavirus long-haulers, if there’s any silver lining to this situation it’s the possibility that out of COVID-19 we’ll get a better understanding of ME/CFS, with the potential benefit for both communities,” he said.
While that may be a silver lining, it’s one that will put the healthcare systems of hard-hit countries under pressure going forward.
“[With] other recent coronavirus outbreaks, some studies showed 20 to 25 per cent of patients also went on to have long-term symptoms,” Mr Amitay explained.
Even if that does turn out to be lower among COVID-19 patients, in a country like the US which has already recorded more than 5 million known cases, that still represents many hundreds of thousands of potential long-haulers who will battle symptoms with no end in sight.
“The fact that the numbers are so large, the implications to the healthcare system ... they’re very scary,” he said.
Do you have a story tip? Email: newsroomau@yahoonews.com.
You can also follow us on Facebook, Instagram and Twitter and download the Yahoo News app from the App Store or Google Play.





