Covid Is Surging Right Now. Here's What Alarms Doctors The Most.

We don’t typically associate hot weather with viral illnesses, but COVID has thwarted that in recent years. This summer seems to be no exception: Recent data from the Centers for Disease Control and Prevention shows that COVID test positivity rates and emergency room visits are steadily rising, especially along both coasts.
The culprit: the FLiRT variants. This family of variants, which evolved from omicron, took off in the spring. Now, they account for over 50% of infections.
According to Dr. Robert H. Hopkins, Jr., the medical director of the National Foundation for Infectious Diseases, this year’s summer wave got an early start ― and it doesn’t appear to be slowing down anytime soon. “I suspect it’s going to increase,” Hopkins told HuffPost. “It seems like we’re seeing more and more states showing increased levels of activity.”
Here’s what to know about the summer COVID spike:
What’s up with the new FLiRT variants?
The FLiRT variants are offshoots of JN.1, which was the dominant variant in the U.S. this past winter.
This family of variants appears to be very contagious, thanks to mutations in the spike protein that may improve the virus’s ability to bind to human cells. “When we look at their molecular profile, some of those mutations potentially could allow the [virus] to escape from previous immunity,” Hopkins explained.
According to Dr. Nikhil Bhayani, an assistant professor in the department of internal medicine at the Burnett School of Medicine at Texas Christian University, one variant in particular is gaining steam right now: KP.3. It’s currently responsible for roughly 25% of cases.
Two other variants in the FLiRT family, KP.2 and KP.1.1, make up 22.5% and 7.5% of infections, respectively. Research from Japan found that KP.2, the dominant variant this past spring, was more transmissible than its predecessors and potentially better at outsmarting our vaccines.
Fortunately, it doesn’t seem like the illness will be any different with the FLiRT variants, according to Hopkins. He suspects they’ll trigger the typical COVID symptoms: Fever, cough, congestion, sore throat, body aches and, though less common these days, loss of taste and smell.
The increase in cases also doesn’t appear to be causing an uptick in hospitalizations. “There’s no evidence they’re more severe than what we’ve been dealing with,” Hopkins said.
What concerns experts about this wave of infections?

We’ve seen summertime increases in COVID infections every year during the pandemic, according to Hopkins, so this isn’t too out of the ordinary. What does alarm him, however, is how early we’re seeing the summer wave kick off this year.
According to Aubree Gordon, a professor of epidemiology and director of the Michigan Center for Infectious Disease Threats & Pandemic Preparedness in the School of Public Health at the University of Michigan, variants gain traction when they evolve to evade the immunity we achieved through past infections and vaccinations.
The current wave is “probably predominately [caused] by those changes in the virus that are probably resulting in it being able to better get around preexisting immunity,” Gordon told HuffPost.
It doesn’t help that it’s likely been a while since many people were last vaccinated. In May, the CDC revealed that only 22% of adults had received an updated COVID shot since it was released in September 2023.
This dip in immunity, combined with the FLiRT variants’ advantageous mutations, could be fueling the spread. Recent gatherings marking the start of summertime, including Memorial Day Weekend and Father’s Day, may be contributing, too, according to Hopkins. It’s known, after all, that social gatherings are a huge source of disease transmission.
Is now a good time to get a booster shot?
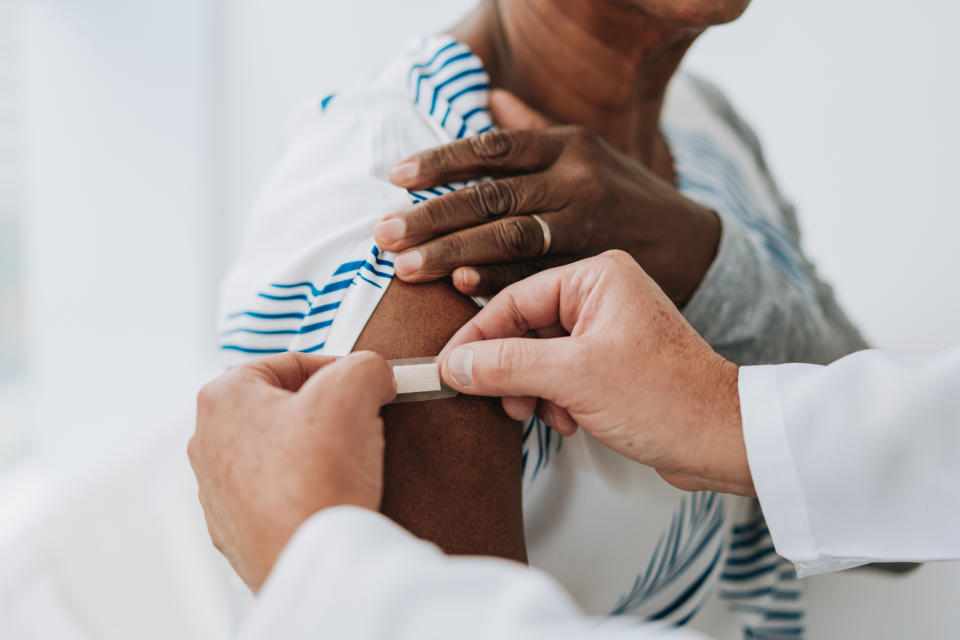
It’s expected that all main vaccine manufacturers will have an updated shot available in the fall that, most likely, will target the KP.2 strain. If you’re wondering whether you should get another jab now or hold off until the new booster’s here, know this: There’s really no wrong time to get a booster shot, Bhayani said.
While the updated shot will likely better target circulating strains, the currently available vaccines will likely still provide good protection against getting sick, and more important, winding up in a hospital or dying, research suggests.
The timing of your next dose depends on your overall health and when you got your previous booster or were last infected. In general, health experts recommend spacing doses out by at least four months.
If you were infected or got vaccinated in the past few months, it might make the most sense to hold off until the new shot’s out later this year, Gordon said. “I’d recommend they delay vaccination just because they’re not going to benefit from it too much at this point,” she said.
That said, Hopkins recommends that people 65 and older who didn’t receive the latest vaccine to go out and get another shot now. The same goes for people who are immunocompromised and haven’t had a shot in the past two months.
“Why take a chance with this current surge if we’ve got something that is going to reduce your severity of illness?” Hopkins said.
Here’s what to do if you get COVID this summer.

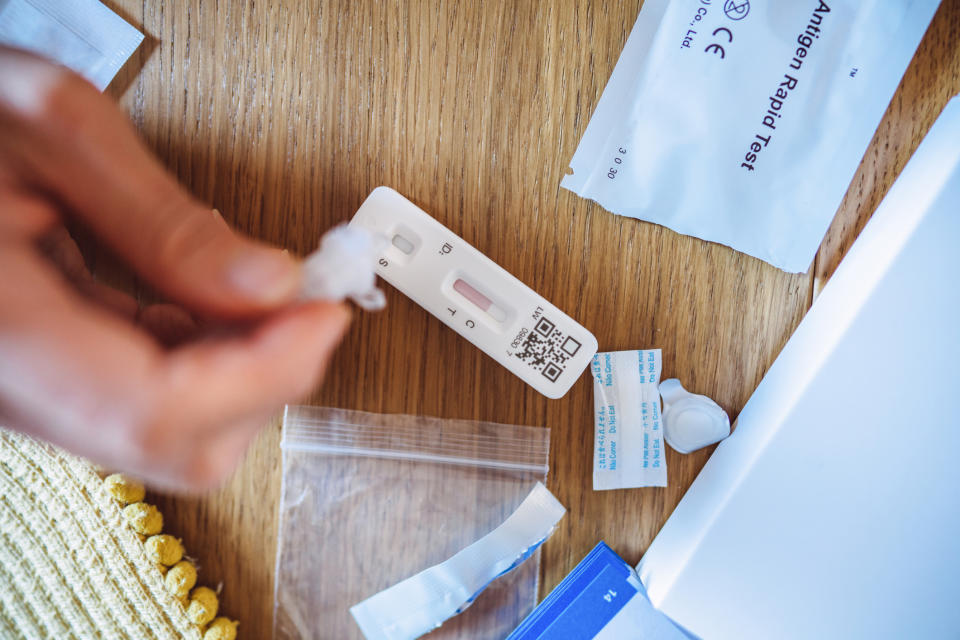
If you contract COVID, it’s a good idea to first test yourself at home with an antigen test. If your test is negative, Hopkins recommended testing yourself again in 24 hours because it can take a few days for the virus to become detectable in your sinuses.
If you’re concerned about your symptoms, reach out to your primary care physician or visit an urgent care to get a PCR test ― these are more sensitive and catch a higher percentage of cases.
Older adults, people who are immunocompromised and those with chronic illnesses face a higher risk of severe disease. Hopkins advised anyone in these groups to contact a health care provider as soon as they feel sick. There are effective oral antivirals ― Paxlovid and molnupiravir ― that can shorten the duration of your illness and reduce the severity of it. But here’s the kicker: They work best when given within five days after symptoms appear.
As for otherwise healthy individuals who test positive, the same tried-and-true measures still work well. Acetaminophen and anti-inflammatories, like ibuprofen and naproxen, can reduce a fever, nasal sprays alleviate congestion, drinking fluids prevents dehydration and getting plenty of rest will aid your overall recovery, Hopkins said.
Finally, keep a distance from other people for five days or until your symptoms are improving. If you do go out, the CDC recommends masking up until the 11th day of your sickness.
These new variants might be adept at skirting our immunity, but getting another booster shot and wearing a high-quality mask in crowded spaces are still the very best ways to stay healthy this summer.This article originally appeared on HuffPost.


