Country’s quiet coronavirus crisis after devastating first wave
Few countries have allowed the novel coronavirus to run as rampant as India – and now the country of more than 1.3 billion people faces a serious post-Covid health crisis.
Health experts are warning that the country’s healthcare system will struggle to deal with those suffering the long-terms side-effects of Covid, which in some cases can be debilitating for many months after being diagnosed with the disease.
Tens of thousands of people across the world have been reporting post-Covid health complications, in a growing community known as coronavirus long-haulers, who deal with a multitude of post viral symptoms including fever, aches and pains, fatigue, chest pain, hair loss, brain fog, nausea and much more.
Despite implementing a range of now-discarded lockdown measures, India failed to get its first wave of the coronavirus under control. As such the country is still very much preoccupied with dealing with the initial onslaught of the virus, but there is a growing number of people who are requiring post-Covid hospital treatment.

Suresh Kumar got a new job as a salesman after recovering from Covid, but was soon unable to work after suffering from fatigue, leg pain and an inability to concentrate.
Sharing his story with the BBC, he explained how he tried to push through the symptoms until he collapsed and his wife later took him to a hospital where the doctor told him about thrombosis.
Thrombosis occurs when a blood clot forms in one or more of the deep veins in your body, usually in your legs, and has emerged as a potentially deadly symptom among coronavirus long-haulers. Mr Kumar’s condition was indeed life-threatening, the BBC reported.
"I was so surprised. I thought I had managed to beat Covid-19. I had to rest for four weeks and I lost my job. I still feel weak but thankfully I have managed to get another job that doesn't require travelling,” he told the broadcaster.
'A life sentence': The frightening trend emerging in young coronavirus patients
'I cannot function': NSW woman tests positive for coronavirus three times
Mr Kumar's story is common in India, which has a massive workforce in the informal sector where millions work as daily-wagers, which often involves hard physical labour and little rest. For those still recovering from the virus, that can be a recipe for disaster.
Health experts are warning that the country needs to focus more on post-Covid care, after tallying more than 6 million official cases of coronavirus to date. Only the US has more.
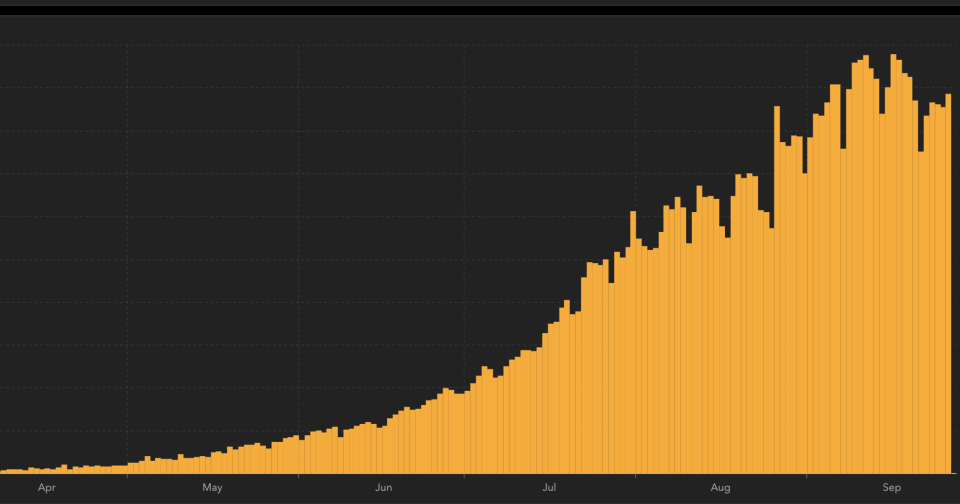
Even in countries with a more advanced healthcare system, post-Covid care is becoming a major concern.
Oved Amitay, the CEO of the Solve ME/CFS Initiative, has seen first-hand how virus patients can go on to develop chronic symptoms that require ongoing medical help and treatment.
“[With] other recent coronavirus outbreaks, some studies showed 20 to 25 per cent of patients also went on to have long-term symptoms,” he told Yahoo News Australia in August.
Even if that does turn out to be lower among COVID-19 patients, in countries like the US and India, that still represents many hundreds of thousands of potential long-haulers who will battle symptoms with no end in sight.
“The fact that the numbers are so large, the implications to the healthcare system ... they’re very scary,” he said.
India’s social inequalities reflected in coronavirus care
When Pradeep Kumar’s wife was admitted to a government-run hospital in India’s capital for treatment of COVID-19, it took two days before she was able to see a doctor.
“There are six other women in her room and everyone is frustrated,” he said outside New Delhi’s LNJP Hospital.
“They’re behaving like they’re leprosy patients.”

Kumar’s wife had just given birth when she found out she had the virus. She was told she would have to change hospitals and be admitted at one set up to handle coronavirus patients, an exhausting process that took hours.
Though India’s leaders have promised coronavirus testing and care for all who need it, regardless of income, treatment options are as stratified and unequal as the country itself. Care ranges from crowded wards at public hospitals that some worry will make them sicker than if they stayed home to spacious suites at private hospitals that only the wealthy can afford.
Under India’s health care system, everyone should be able to receive either free or highly subsidised care at those public hospitals depending on their income. But the system has been chronically underfunded, meaning government hospitals are overburdened and patients often face days-long waits for even basic treatments.
World Health Organisation data shows that India’s government spent $63 per person on health care for its 1.3 billion people in 2016. By comparison, China spent $398 for each of its 1.4 billion people in 2016, according to the WHO.
Though India has managed to halve its poverty rate over the past 15 years, some 176 million people still live on less than $AUD2.50 a day, and experts say the pandemic is shining a spotlight on the country’s vast inequalities in everything from employment rights to health care.
The two-tiered hospital system is having an impact even beyond the coronavirus.
Vishnu Singh’s 14-year-old daughter has had a fever and fallen unconscious every night for a month. But given the current situation at public hospitals, he wouldn’t dare take her to one.
“The public hospitals are full of people with the virus,” he said.
“You could get infected just standing in line.”
Instead he’s spent 10,000 rupees (AUD$192) — two-thirds of his monthly income as an office manager — to have exams and tests done at private hospitals and labs. It’s still not clear what’s causing his daughter’s sickness.
with AP
Do you have a story tip? Email: newsroomau@yahoonews.com.
You can also follow us on Facebook, Instagram and Twitter and download the Yahoo News app from the App Storeor Google Play.





