4 Common Misconceptions About Cervical Screenings That We All Need To Unlearn
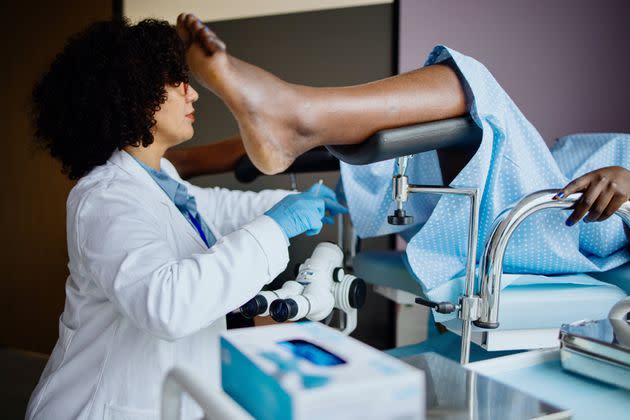
According to data from NHS England, about 4.6 million people aged 25 to 64 in England (or 30%) have never been screened for cervical cancer or haven’t taken up their latest invitation to book appointments for screenings.
However, early screening is more important than ever, with cancer charity Macmillan Cancer Support revealing that the cancer survival rates in the UK are 25 years behind other European countries.
Dr Rosie Godeseth, Associate Medical Director at Vitality believes that some of the misconceptions that we have about cervical screening tests (smear tests) are behind the falling rates of uptakes.
Common myths about cervical screenings
Myth: Cervical screening is always very painful
Dr Godeseth said: “Cervical screening should not hurt. It might feel a little strange or uncomfortable, but it should not be painful. If you’re worried speak to your doctor as there are different things they can do to make the process more comfortable for you.”
For people with gynaecological health conditions or tilted cervixes, smears can be quite sore.
Jo’s Cervical Care advises that the most common way to make this more comfortable for you is to ball your fists up and then put them under your bum when you’re getting a test.
This makes your bum higher so that your sample taker can get a better view of your cervix.
Myth: You don’t need to be screened if you’ve had the HPV vaccine
Reality: The HPV vaccine does a great job at preventing cases of cervical cancer, however, it does not protect against every type of HPV which is why it’s so important to have a smear test when invited to do so.
Myth: Cervical screening is only for people who have had sex
Reality: Some believe cervical cancer is solely caused by sex and as such you only need a smear test if you have had sex. This is a myth, and you should still be screened as there is still a risk of developing cervical cancer.
Myth: An abnormal result means you have cancer
Dr Godeseth said: “An abnormal test result does not mean cancer, so you don’t need to jump to worst-case scenarios in your mind. Instead, an abnormal result means you have changes in the cells covering your cervix.
“These can sometimes go back to normal by themselves or it may develop into cancer if left untreated. Where you receive an abnormal result, your doctor will work with you to discuss what this means and what the next steps are for you.”
How to advocate for yourself when getting a smear test
For some people, it’s not just as simple as gritting your teeth and getting through an appointment. Chronic pain conditions and sexual trauma can make cervical screenings more than just another appointment.
Macmillan Cancer Support advised: “If you are finding it difficult to cope, but you want to have the test, it may help to talk about it with someone.
“You may want to talk to a friend or family member. Your GP or practice nurse can answer any questions you have and explain ways they can make the test easier for you.”
You can also request that a loved one comes with you for the test so that you have familiar support as it happens.
Additionally, Eve Appeal have created a guide for survivors of sexual abuse who are apprehensive about cervical smears.
How to get a smear test
The NHS stated: “You’ll be sent an invitation letter in the post when it’s time to book your cervical screening appointment. Your invitation letter will tell you where you can go for cervical screening and how to book.
“Most cervical screening is done in a GP surgery by a female nurse or doctor. Call your GP surgery to book an appointment with them. You might be able to book the appointment online.”

